 Kostadin Kostadinov, Ivelina Popova-Sotirova, Yuliyana Marinova, Nina Musurlieva, Georgi Iskrov and Rumen Stefanov, as part of the Institute for Rare Diseases and Medical University – Plovdiv examine the availability and access to orphan drugs for rare cancers in Bulgaria, aiming to respond to the need for its improvement. This research provides valuable insights into the challenges faced by patients with rare cancers in accessing treatment and has been published in the prestigious international journal “Cancers” (Impact factor: 5.2).
Kostadin Kostadinov, Ivelina Popova-Sotirova, Yuliyana Marinova, Nina Musurlieva, Georgi Iskrov and Rumen Stefanov, as part of the Institute for Rare Diseases and Medical University – Plovdiv examine the availability and access to orphan drugs for rare cancers in Bulgaria, aiming to respond to the need for its improvement. This research provides valuable insights into the challenges faced by patients with rare cancers in accessing treatment and has been published in the prestigious international journal “Cancers” (Impact factor: 5.2).
Rare cancers are defined by an annual incidence of fewer than 6 per 100,000. Bearing similarities to rare diseases, they are associated with substantial health inequalities due to diagnostic complexity and delayed access to innovative therapies. This situation is further aggravated in Southeastern European countries like Bulgaria, where limited public resources and expertise underscore the need for additional policy and translational research on rare cancers.
This study aims to explore the availability and access to orphan drugs for rare cancers in Bulgaria for the period of 2020–2023. The data from both the European Union and national public sources is cross-compared to evaluate the number of available and accessible orphan drugs for rare cancers, the delay from market authorization to reimbursement, the dynamics of public expenditures, and regional disparities in access across the country. The main characteristics of oncological and non-oncological orphan drugs are juxtaposed as well.
Only 15 out of 50 oncological orphan drugs that were authorized by the European Medicine Agency were accessible for rare cancer patients in Bulgaria. The median external delay defined as the time interval between EMA authorization and PDL inclusion of the respected cancer orphan drugs was 760 days. The total expenditures for all orphan drugs for rare cancers amounted to EUR 74,353,493 from 2020 to 2023. The budgetary impact of this group rose from 0.24% to 3.77% of total public medicinal product expenditures for the study period.
Rare cancer patients represent a vulnerable population that often faces limited to no access to treatment. This article calls for targeted European and national policies to address this major inequality. Read the full article here.

 Sarcoidosis is a chronic inflammatory granulomatous disease of unknown cause. Delays in diagnosis can result in disease progression. The aim of this study is to review the current literature and determine the overall diagnostic delay of sarcoidosis, factors associated with diagnostic delay, and the experiences of people with sarcoidosis of diagnostic delay.
Sarcoidosis is a chronic inflammatory granulomatous disease of unknown cause. Delays in diagnosis can result in disease progression. The aim of this study is to review the current literature and determine the overall diagnostic delay of sarcoidosis, factors associated with diagnostic delay, and the experiences of people with sarcoidosis of diagnostic delay. Ralitza Raycheva, Kostadin Kostadinov, Georgi Iskrov, Georgi Stefanov, Elena Mitova and Rumen Stefanov, as part of the Institute for Rare Diseases and the Department of Social Medicine and Public Health at the Medical University – Plovdiv, actively participate in the Screen4Care project, which started in 2021. Screen4Care offers an innovative research approach to accelerate rare disease diagnosis, which is based on two central pillars: genetic newborn screening and digital technologies.
Ralitza Raycheva, Kostadin Kostadinov, Georgi Iskrov, Georgi Stefanov, Elena Mitova and Rumen Stefanov, as part of the Institute for Rare Diseases and the Department of Social Medicine and Public Health at the Medical University – Plovdiv, actively participate in the Screen4Care project, which started in 2021. Screen4Care offers an innovative research approach to accelerate rare disease diagnosis, which is based on two central pillars: genetic newborn screening and digital technologies.
 Newborn screening plays a crucial role in early detection of conditions in newborns. This leads to timely therapeutic interventions that can significantly improve outcomes. Ensuring quality and standardization of newborn screening procedures is crucial for its effectiveness. We had the privilege to interview Peter Schielen, Director of the International Society for Neonatal Screening (ISNS) office, an expert in quality issues and standardization of neonatal screening, and Editor-in-Chiefof the scientific journal “International Journal of Neonatal Screening”. Peter Schielen is a guest lecturer at the 10th International Symposium on Health Technology Assessment (5.04.2024 in Sofia) by invitation of the Institute for Rare Diseases.
Newborn screening plays a crucial role in early detection of conditions in newborns. This leads to timely therapeutic interventions that can significantly improve outcomes. Ensuring quality and standardization of newborn screening procedures is crucial for its effectiveness. We had the privilege to interview Peter Schielen, Director of the International Society for Neonatal Screening (ISNS) office, an expert in quality issues and standardization of neonatal screening, and Editor-in-Chiefof the scientific journal “International Journal of Neonatal Screening”. Peter Schielen is a guest lecturer at the 10th International Symposium on Health Technology Assessment (5.04.2024 in Sofia) by invitation of the Institute for Rare Diseases. 10th INTERNATIONAL SYMPOSIUM
10th INTERNATIONAL SYMPOSIUM The integration of whole genome sequencing into all aspects of modern medicine represents the next step in the evolution of healthcare. Using this technology, scientists and physicians can observe the entire human genome comprehensively, generating a plethora of new sequencing data. Modern computational analysis entails advanced algorithms for variant detection, as well as complex models for classification. Data science and machine learning play a crucial role in the processing and interpretation of results, using enormous databases and statistics to discover new and support current genotype-phenotype correlations.
The integration of whole genome sequencing into all aspects of modern medicine represents the next step in the evolution of healthcare. Using this technology, scientists and physicians can observe the entire human genome comprehensively, generating a plethora of new sequencing data. Modern computational analysis entails advanced algorithms for variant detection, as well as complex models for classification. Data science and machine learning play a crucial role in the processing and interpretation of results, using enormous databases and statistics to discover new and support current genotype-phenotype correlations.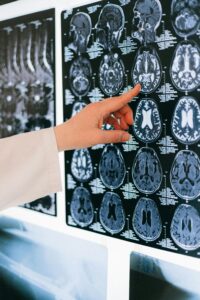 Benign tumors, called vestibular schwannomas, originate from the eighth cranial nerve and have a variable natural history. Clinically and radiologically, the solid variety is distinguished from cystic vestibular schwannomas (VS) forms, a rare benign subgroup.
Benign tumors, called vestibular schwannomas, originate from the eighth cranial nerve and have a variable natural history. Clinically and radiologically, the solid variety is distinguished from cystic vestibular schwannomas (VS) forms, a rare benign subgroup. Silver-Russell syndrome (SRS) is a rare disease with an incidence of 1:30,000 to 1:100,000 newborns. Due to apparent clinical heterogeneity, a large proportion of patients with SRS are undiagnosed. The main characteristics of the syndrome are intrauterine retardation and postnatal growth retardation, dysmorphic stigmas, and malformations of other organs and systems.
Silver-Russell syndrome (SRS) is a rare disease with an incidence of 1:30,000 to 1:100,000 newborns. Due to apparent clinical heterogeneity, a large proportion of patients with SRS are undiagnosed. The main characteristics of the syndrome are intrauterine retardation and postnatal growth retardation, dysmorphic stigmas, and malformations of other organs and systems. IgA nephropathy (ORPHA code: 34145) is a rare, serious condition in the complex field of renal diseases. It is an immune-mediated kidney disease that progresses over time. It emerges as a significant contributor to renal failure on a global scale. This article provides new information about this complex renal disorder. It was co-authored by Elena Mitova, MD and Georgi Stefanov, MD from the Institute for Rare Diseases in Plovdiv, and prof. Julian Ananiev of department of General and Clinical Pathology, Forensic Medicine, Deontology and Dermatovenerology, Medical Faculty, Trakia University, Stara Zagora. Their combined efforts create a narrative that clarifies the complex epidemiological environment of IgA nephropathy.
IgA nephropathy (ORPHA code: 34145) is a rare, serious condition in the complex field of renal diseases. It is an immune-mediated kidney disease that progresses over time. It emerges as a significant contributor to renal failure on a global scale. This article provides new information about this complex renal disorder. It was co-authored by Elena Mitova, MD and Georgi Stefanov, MD from the Institute for Rare Diseases in Plovdiv, and prof. Julian Ananiev of department of General and Clinical Pathology, Forensic Medicine, Deontology and Dermatovenerology, Medical Faculty, Trakia University, Stara Zagora. Their combined efforts create a narrative that clarifies the complex epidemiological environment of IgA nephropathy. Paroxysmal nocturnal hemoglobinuria (PNH) is a chronic multisystem, progressive and life-threatening disease which is characterized by intravascular hemolysis, thrombotic complications, severe infections and bone marrow failure. PNH is a rare disease with estimated prevalence of 2/100 000 by Orphanet data.
Paroxysmal nocturnal hemoglobinuria (PNH) is a chronic multisystem, progressive and life-threatening disease which is characterized by intravascular hemolysis, thrombotic complications, severe infections and bone marrow failure. PNH is a rare disease with estimated prevalence of 2/100 000 by Orphanet data.