 We are pleased to announce the 16th Annual ICORD Meeting, a premier event dedicated to advancing knowledge and collaboration in the field of rare diseases. The conference will take place on July 24-25, 2024, in Buenos Aires, Argentina, at the “Aula Magna”, Faculty of Pharmacy and Biochemistry, University of Buenos Aires (UBA). Esteemed professionals and experts in rare diseases from around the world will gather to engage in meaningful discourse and exchange valuable insights.
We are pleased to announce the 16th Annual ICORD Meeting, a premier event dedicated to advancing knowledge and collaboration in the field of rare diseases. The conference will take place on July 24-25, 2024, in Buenos Aires, Argentina, at the “Aula Magna”, Faculty of Pharmacy and Biochemistry, University of Buenos Aires (UBA). Esteemed professionals and experts in rare diseases from around the world will gather to engage in meaningful discourse and exchange valuable insights.
Hosted by ICORD, the International Collaboration for Rare Diseases and Orphan Drugs, and co-hosted by the Faculty of Pharmacy and Biochemistry of the University of Buenos Aires and CERyDH, this meeting emphasizes the importance of implementing comprehensive health programs for rare diseases and developing orphan drugs tailored to Latin American realities. The event also highlights the necessity of prioritizing programs based on local health conditions and fostering collaboration among scientists and the health industry globally.
Program Highlights:
- Day 1: Opening sessions will feature prominent speakers like Emilio Roldan, Pablo Evelson, Cynthia J. Tifft, and Daniel Salamone. Discussions will cover international collaborations in rare disease research, genomic approaches, and innovative therapies.
- Day 2: Sessions will include presentations on rare disease research in Argentina, patient resilience stories, and plenary conferences on rare disease education and international collaboration.
Attendees will benefit from simultaneous Spanish/English translation services, poster sessions, and business lunches aimed at fostering research collaborations. Registration fees are set at 50 Euros, with various grants available for members of UBA, CONICeT, patients, journalists, speakers, and poster presenters.
For more information and to register, visit the official ICORD website (www.icord.es). Join us in Buenos Aires for this significant event to foster excellence and advancements in the understanding and treatment of rare diseases.


 Pulmonary alveolar proteinosis (PAP) is an ultra-rare disease caused by impaired pulmonary surfactant clearance due to the dysfunction of alveolar macrophages or their signaling pathways. PAP is categorized into autoimmune, congenital, and secondary PAP, with autoimmune PAP being the most prevalent. This article aims to present a comprehensive review of PAP classification, pathogenesis, clinical presentation, diagnostics, and treatment. The PAP diagnosis is usually based on clinical symptoms, radiological imaging, and bronchoalveolar lavage, with additional GM-CSF antibody tests. The gold standard for PAP treatment is whole-lung lavage. This review presents a summary of the most recent findings concerning pulmonary alveolar proteinosis, pointing out specific features that require further investigation. Read the full article
Pulmonary alveolar proteinosis (PAP) is an ultra-rare disease caused by impaired pulmonary surfactant clearance due to the dysfunction of alveolar macrophages or their signaling pathways. PAP is categorized into autoimmune, congenital, and secondary PAP, with autoimmune PAP being the most prevalent. This article aims to present a comprehensive review of PAP classification, pathogenesis, clinical presentation, diagnostics, and treatment. The PAP diagnosis is usually based on clinical symptoms, radiological imaging, and bronchoalveolar lavage, with additional GM-CSF antibody tests. The gold standard for PAP treatment is whole-lung lavage. This review presents a summary of the most recent findings concerning pulmonary alveolar proteinosis, pointing out specific features that require further investigation. Read the full article 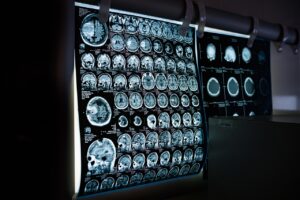 The Angelman Syndrome Registry (Research in Angelman Syndrome in Italy) aimed to assess the clinical history of individuals with Angelman Syndrome in Italy, compare it with existing literature, and explore the link between symptoms and genotypes. Established in 2018, the study enrolled 82 participants, with 62 providing complete data. It collected demographic, clinical, and genetic information using electronic forms, analyzing the data with descriptive statistics and examining genotype-clinical characteristic associations.
The Angelman Syndrome Registry (Research in Angelman Syndrome in Italy) aimed to assess the clinical history of individuals with Angelman Syndrome in Italy, compare it with existing literature, and explore the link between symptoms and genotypes. Established in 2018, the study enrolled 82 participants, with 62 providing complete data. It collected demographic, clinical, and genetic information using electronic forms, analyzing the data with descriptive statistics and examining genotype-clinical characteristic associations. Hereditary fructose intolerance is a rare genetic disorder that is inherited in an autosomal recessive manner, with mutations sometimes occurring spontaneously. This rare disease it with ICD-10 code: E74.1 and
Hereditary fructose intolerance is a rare genetic disorder that is inherited in an autosomal recessive manner, with mutations sometimes occurring spontaneously. This rare disease it with ICD-10 code: E74.1 and  Prenatal diagnoses of congenital malformations have increased significantly due to high-resolution prenatal imaging. However, discussing these diagnoses with expectant parents remains challenging due to the varied outcomes associated with congenital malformations. Comprehensive prenatal genetic testing, including chromosomal microarray, exome sequencing, and genome sequencing, has become essential for improving prognostic accuracy.
Prenatal diagnoses of congenital malformations have increased significantly due to high-resolution prenatal imaging. However, discussing these diagnoses with expectant parents remains challenging due to the varied outcomes associated with congenital malformations. Comprehensive prenatal genetic testing, including chromosomal microarray, exome sequencing, and genome sequencing, has become essential for improving prognostic accuracy. Rare diseases are an often chronic and progressive group of conditions affecting more than 30 million people in Europe. These diseases are associated with significant direct and indirect costs to a spectrum of stakeholders, ranging from individuals and their families to society overall. Further quantitative research on the economic cost for children and their families living with a rare disease is required as there is little known on this topic.
Rare diseases are an often chronic and progressive group of conditions affecting more than 30 million people in Europe. These diseases are associated with significant direct and indirect costs to a spectrum of stakeholders, ranging from individuals and their families to society overall. Further quantitative research on the economic cost for children and their families living with a rare disease is required as there is little known on this topic. Patient registries are crucial for rare disease management. However, manual registry construction is labor-intensive and not user-friendly. The aim of this study is to establish Hong Kong’s first computer-assisted patient identification tool for rare diseases, starting with Inborn errors of metabolism (IEM).
Patient registries are crucial for rare disease management. However, manual registry construction is labor-intensive and not user-friendly. The aim of this study is to establish Hong Kong’s first computer-assisted patient identification tool for rare diseases, starting with Inborn errors of metabolism (IEM). Prader-Willi syndrome (PWS) is a rare disease, which shows a peculiar clinical phenotype, including obesity, which is different from essential obesity (EOB). Metabolomics might represent a valuable tool to reveal the biochemical mechanisms/pathways underlying clinical differences between PWS and EOB. The aim of the present (case-control, retrospective) study is to determine the metabolomic profile that characterizes PWS compared to EOB.
Prader-Willi syndrome (PWS) is a rare disease, which shows a peculiar clinical phenotype, including obesity, which is different from essential obesity (EOB). Metabolomics might represent a valuable tool to reveal the biochemical mechanisms/pathways underlying clinical differences between PWS and EOB. The aim of the present (case-control, retrospective) study is to determine the metabolomic profile that characterizes PWS compared to EOB. The Dyke-Davidoff-Masson syndrome (DDMS) is an uncommon neurological disorder whose prevalence is not yet known. There have only been 21 adult manifestations of this rare brain disorder, out of around 100 cases previously documented. Diagnosis is challenging because of the complexity of radiological findings and clinical symptoms, which include ventricle dilation, hypertrophy of the cranial bones, increased pneumatization of the sinuses, and cerebral hemisphere atrophy. It can be inherited or acquired from infections, brain hemorrhage, and hypoxia during pregnancy. Usually, neuroimaging is used to diagnose it. This case study reports the case of a 17-year-old girl who had complex partial seizures at the age of 17 and right-side paralysis since she was three years old. Read the full article
The Dyke-Davidoff-Masson syndrome (DDMS) is an uncommon neurological disorder whose prevalence is not yet known. There have only been 21 adult manifestations of this rare brain disorder, out of around 100 cases previously documented. Diagnosis is challenging because of the complexity of radiological findings and clinical symptoms, which include ventricle dilation, hypertrophy of the cranial bones, increased pneumatization of the sinuses, and cerebral hemisphere atrophy. It can be inherited or acquired from infections, brain hemorrhage, and hypoxia during pregnancy. Usually, neuroimaging is used to diagnose it. This case study reports the case of a 17-year-old girl who had complex partial seizures at the age of 17 and right-side paralysis since she was three years old. Read the full article  Extramammary Paget’s disease (EMPD) is a rare cancer that occurs within the epithelium of the skin, arising predominantly in areas with high apocrine gland concentration. The aim of this article is to integrate clinicopathological data with genomic analysis of aggressive, rapidly-progressing de novo metastatic EMPD responding to HER2-directed treatment in combination with other agents, to attain a more comprehensive understanding of the disease.
Extramammary Paget’s disease (EMPD) is a rare cancer that occurs within the epithelium of the skin, arising predominantly in areas with high apocrine gland concentration. The aim of this article is to integrate clinicopathological data with genomic analysis of aggressive, rapidly-progressing de novo metastatic EMPD responding to HER2-directed treatment in combination with other agents, to attain a more comprehensive understanding of the disease.